Blood Groups-ABO Blood Group and Rh Group System
Blood is an important fluid within the body, as it transports oxygen, nutrients, and waste. It is comprised of plasma, red and white blood cells and platelets. The two blood group systems in identifying compatibility in blood transfusions are the ABO system with the four types being A, B, AB, and O, and the Rh factor, which could either be positive or negative. Around 85% of the people are Rh-positive, and O-positive is the most common blood type worldwide. The ABO system of blood grouping and the Rh factor comes under the basics of biology which is important for several major chapters of human physiology.
Don't Miss: Most scoring concepts for NEET | NEET papers with solutions
NEET 2025: Syllabus | PYQs | Crack NEET in 2 months - Study Plan
NEET Important PYQ & Solutions: Physics | Chemistry | Biology | NEET PYQ's (2015-24)
- Blood Group
- Who Discovered Blood Group?
- What are ABO and Rh blood groups?
- Diagnostic Testing for Blood Groups
- Principles of Blood Grouping

Blood Group
The term blood type or blood group refers to the division of blood based on the absence or presence of antibodies and hereditary antigenic substances on the surface of RBCs.
Based on the blood group system, these antigens may be proteins, carbohydrates, glycoproteins, or glycolipids. Many additional cell types seen in other organs also have some of these antigens on their surfaces. These red blood cell surface antigens that make up a blood group system can all originate from the same allele (or different gene).
The two most important blood group coding schemes are ABO and Rh, they specify a person's blood type for compatibility with blood transfusions.
Read more
- Practice MCQ on the Blood Group System
- Body Fluids And Circulation
- Human Heart
- Excretory Products And Their Elimination
Who Discovered Blood Group?
- In 1901, Karl Landsteiner discovered the AB blood type.
- He found in 1900 that when red blood cells and serum from a different person are combined in a test tube, the red blood cells agglutinate.
- The blood groups A, AB, B, and O were discovered and given names in 1909.
- In 1930, he was awarded the Nobel Prize.
- There are three different blood groups, A, B and O, according to the AB blood group, based on whether antigens A, B and O are present or not.
Diagram of Types of blood groups
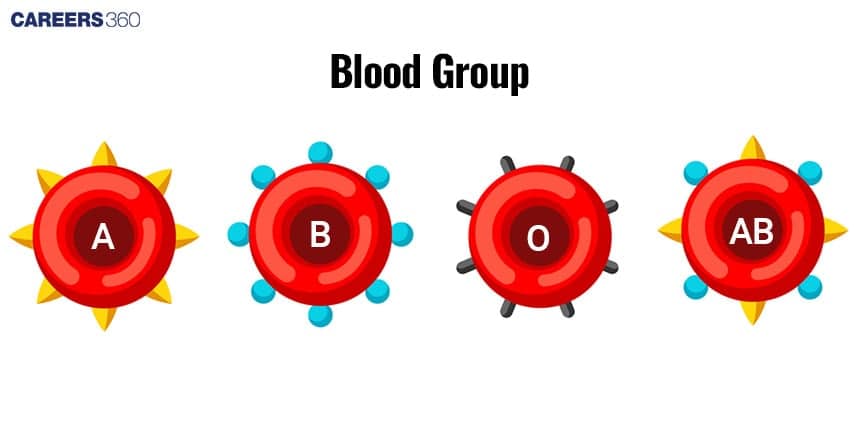
What are ABO and Rh blood groups?
ABO and Rh blood groups are two systems that classify human blood according to the existence of specific proteins in red blood cells. The ABO system classifies blood into four types: A, B, AB, and O, according to the kind of antigens found on the cells. The Rh system determines whether the blood is positive if the Rh factor protein is present, or negative if it is absent. Together, they are crucial in safe blood transfusion and for the understanding of blood compatibility.
ABO Blood Group System
The ABO blood group system is one of the most important blood type systems in human biology, identified by Karl Landsteiner in 1901.
Basics of ABO Blood Groups
Antigens: proteins on the surface of RBCs that determine blood type.
Antibodies: Proteins in plasma reacting against the foreign antigens.
Four basic blood types: A (A antigen), B (B antigen), AB, and O (no A or B antigens).
Immune Reactions Between Antigens and Antibodies
Antigens A and B establish blood type based on the presence or absence of specific antibodies.
Agglutination is the clumping of red blood cells when there is a mixing of incompatible blood types, aggregating dangerous reactions.
Genetics of ABO Blood Groups
Inheritance patterns are Mendelian, A and B are dominant, and O is recessive.
The genotypes AA or AO give type A, BB or BO gives type B, AB gives type AB, and OO gives type O.
Types of ABO Blood
- O-positive: O-positive blood is the blood type accounting for about 35% of our blood donors. Both O-positive and O-negative blood donors can donate blood to individuals with O-positive blood.
- O-negative: A little more than 13% of our blood donors are O-negative. Comparatively, 35% of donors have blood that is O-positive. Since anyone can receive red blood cells from an O-negative donor's gift, this type of donor is frequently referred to as a "universal donor."
- A-positive: A-positive blood is present in about 30% of donors, making it the second most prevalent blood type after O-positive (36%). People with A-positive blood and AB-positive blood can receive A-positive red blood cells.
- A-negative: Only 8% of donors have blood that is A-negative. Comparatively, 30% of donors have blood that is A-positive.
- B-positive: As a result, only 8% of donors have blood that is B-positive. Blood group B is one of the least prevalent blood groups, with only 10% of the population having it. People with B-positive blood and B-positive blood can receive B-positive red blood cells.
- B-negative: Only 2% of our blood donors have B-negative blood. Comparatively, the most prevalent kind of blood, O-positive, is present in 36% of donors. Red blood cells from B-negative donors are available for about 1 in 8 patients.
- AB-positive: One of the rarest blood types in the nation, AB-positive blood is only present in 2% of donors. Only individuals with AB + blood can be treated with red blood cells.
- AB-negative: Only 1% of our blood donors are AB-negative, the rarest blood type in the ABO blood group. Only 3% of all donors are in the AB blood group.
Diagram showing Genetics of Blood Group Inheritance
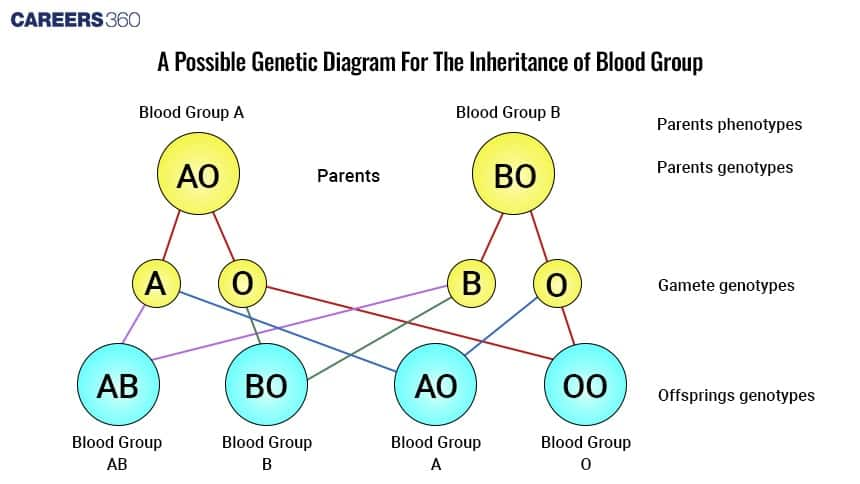
Clinical Significance
Blood transfusions: The knowledge of the blood groups to avoid an immune response.
Organ transplant: Donor–recipient matching of their blood group to avoid organ rejection.
Diagram of ABO Blood Group Compatibility
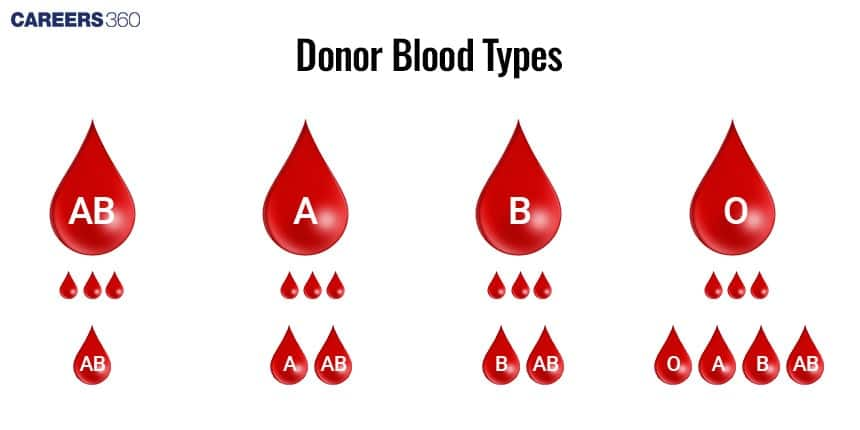
Distribution of the Blood Groups
While Type O is the most frequent in populations all over the world, frequencies of other blood groups vary in different regions.
Differences are prominent in populations and ethnic groups.
Rh Blood Group System
Another critical factor in blood grouping was introduced by Landsteiner and Wiener in 1940, the Rh blood group system.
Diagram of Rh Blood Group System
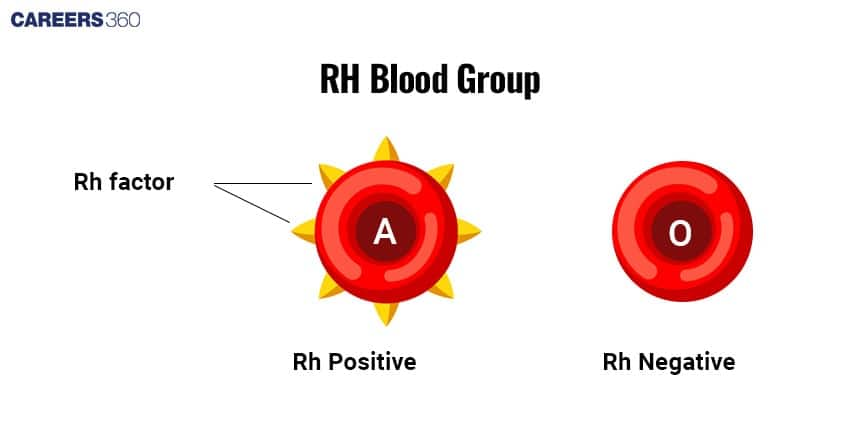
Rh Blood Groups Basics
Rh factor: D antigen is a protein present (+) or absent (-) on some RBCs.
Rh-positive: Presence of D antigen.
Rh-negative: Absence of D antigen.
Genetics of Rh Blood Groups
Inheritance of the D antigen is dominant.
DD or Dd is Rh positive and dd is Rh negative.
Clinical Significance
Blood transfusions: Importance of Rh compatibility.
Hemolytic disease of the newborn: This is a condition whereby an Rh-negative woman is carrying an Rh-positive fetus.
Prevention: Rh immunoglobulin therapy for Rh-negative mothers.
Rh Blood Group Distribution
Global distribution More or less 85% of the population is Rh-positive, though different in various ethnic groups and geographical areas.
High incubation of Rh-negative persons in some populations, like Caucasians.
Diagnostic Testing for Blood Groups
The typing of blood groups requires precision in many aspects linked to medical procedures.
Blood Type Determination Methods
Sliding test: one of the simplest and fastest methods in which only drops of blood and several antibody solutions drop onto the surface of a slide are required.
Tube test: more accurate, mixing blood with antibodies in a test tube.
Gel card test: This is a more accurate and clear blood typing system using gel matrices.
Advanced Diagnostic Techniques
Molecular techniques: PCR-based assays for accurate genetic determination of blood type
Automation: Modern machines for high-throughput, accurate blood typing.
What is an Antigen?
Immunogens, also known as antigens, are toxins or compounds in your blood that cause your body to fight them.
Antigens can be various substances from outside your body that provide a health risk. However, they are typically bacteria or viruses. The immune response is the name given to this conflict. Our body's lymphocytes, or disease-fighting white blood cells, are activated in the presence of antigens. Due to the presence of antigens, white blood cells produce immune system defences termed antibodies.
Types of Antigen
Autoantigens and hetero antigens are the two main types of antigens:
Hetero Antigens are substances made by or found in bacteria, viruses, protozoa, other people's blood and red blood cells, snake venom, allergens like pollen, and certain proteins in food. They are compounds that are foreign to your body.
Our body produces autoantigens, also known as self-antigens, to fight your cells, and they are typically a symptom of a disease such as an autoimmune ailment.
What is an Antibody?
Immunoglobulins, or Ig, are another name for antibodies. They are Y-shaped proteins produced by B lymphocytes or B cells in your immune system.
Viruses and other toxins from the outside are attacked and removed by B cells. Making particular antibodies for a specific sort of antigen allows them to achieve this.
These specialised antibodies bind to and mark their unique antigens for the attack. Additionally, antibodies block these antigens, preventing them from damaging your healthy cells.
Types of Antibodies
Immunoglobulins, or antibodies, come in several main categories:
IgG: These are the antibody subtypes that are most prevalent in plasma. They purify dangerous drugs and offer ongoing security.
IgM: The B cells' initial antibodies produced in response to antigens are these.
IgA: Antigens are gathered by these antibodies and eliminated from the body through mucus or other bodily fluids.
IgE: These antibodies elicit allergies and offer parasite defence. Your skin, lungs, and mucosal membranes all contain trace quantities.
IgD: By attaching to B cells, these antibodies trigger the release of IgM antibodies.
Principles of Blood Grouping
The agglutination reaction is the basis for the ABO and Rh blood categorisation systems. Red blood cells that contain one or both of the antigens interact with one another when they are exposed to the appropriate antibodies to produce visible clumping or agglutination.
The O-linked glycoproteins that make up the ABO blood group antigens are A or B antigens, depending on the terminal sugar residues that are visible on the red blood cell surface.
RBCs from individuals with A antigens and serum anti-B antibodies are both present. People with blood group B also have anti-A antibodies in their serum and B antigens in their RBCs.
People with blood group AB have both A and B antigens on their RBCs but neither A nor B antibodies in their serum. In contrast, people with blood group O have both anti-A and anti-B antibodies in their serum but neither A antigens nor B antigens. The exposed loops on the surface of red blood cells connect with the matching antibodies through transmembrane proteins known as Rh antigens.
Also Read
Recommended Video on Blood Groups
Frequently Asked Questions (FAQs)
The ABO blood group system distinguishes between A and B antigens, while that for Rh is based on the absence of the D antigen.
It is done because different blood types react when combined with certain specific antibodies. This implies that blood typing is very important in transfusions and transplants to ensure that there is compatibility.
No, a person's blood type is genetically determined and remains the same all one's life.
If one were given some wrong blood group, that would have led to serious immune responses, agglutination, and hemolysis, serious and at times fatal.
Rh incompatibility may result in hemolytic disease in the newborn. In fact, until recently, Rh incompatibility between mother and fetus caused such diseases that were invariably prevented by Rh immunoglobulin therapy.
Also Read
29 Nov'24 01:19 PM
27 Nov'24 07:39 PM
27 Nov'24 07:15 PM
27 Nov'24 05:11 PM
26 Nov'24 08:14 PM
26 Nov'24 06:50 PM
26 Nov'24 05:51 PM
26 Nov'24 04:44 PM
26 Nov'24 03:52 PM
26 Nov'24 02:55 PM